YOURS QUESTIONS ABOUT FUNGAL NAIL INFECTIONS
What is fungal nail infection ?
What causes fungal nail infections ?
How does one get fungal nail infection ?
One can get dermatophytes by walking barefoot in damp public places (swimming pools, saunas, cloakrooms, dance halls, tatamis of judo halls, theatre stages, etc…). People infected with dermatophytes will leave fragments of infected skin on the ground and in turn contaminate other people.
Yeasts
Proliferates under the nails of people overexposed to moisture (excessive hand washing, food and catering professionals, health care professionals, day care centre staff, etc.). In fact, in these cases, infection results from detrimental habits which will have to be changed.
Moulds
Walking barefoot on earth soil (garden and forest soils) is a risk factor for catching moulds.
Who is at risk of getting fungal nail infection ?
What are the risk factors ?
Family predisposition.
Some doctors believe there is a genetic predisposition to fungal nail infections.
Some diseases and medication:
– Certain diseases (AIDS, diabetes, Cushing’s Syndrome, etc…) or drugs (immunosuppressive treatments, chemotherapy, treatments against graft-versus host-reaction, cortisone…) promot infections.
– Blood circulation disorders (varicose veins in the legs, pallor of fingers and toes during winter time).
– Certain genetic diseases like Down Syndrome.
– Skin conditions leading to a separation of the nail from the nail bed or to thickened nails (psoriasis, lichen).
– Feet problems leading to a separation of the nail from the nail bed or to thickened nails
Abnormal toe position (toes which overlap, a big toe that is raised or “sticks up”….)
“Blows” and haematoma due to some sports or poorly fitting shoes.
– Life-style related or environmental factors
Moisture, excessive perspiration and continuous wearing of closed shoes. Trades and professions involving the wearing of sports or safety shoes are greatly exposed to the risk of tinea pedis. Professions overexposed to water and/or food also are likely to be exposed to the risk of hand mycosis (tinea manum).
Walking barefoot in public places, in particular in the context of sports and leisure activities.
– Age-related factors. Frequency of fungal nail infections increases with age because nail growth slows down with age but also because of blood.
What are the symptoms of fungal nail infections ?
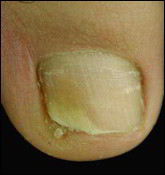
In the beginning, the fungal infection is limited to one or several toenails. The fungus initially contaminates the skin of the interdigits. A crack is then formed that will not go away. This crack generally sits between the fourth and fifth toe, sometimes between the third and the fourth. This often occurs several months or years before nails themselves are contaminated, usually beginning at the corner of the big toenail. At the beginning, nail contamination may result in the following symptoms:
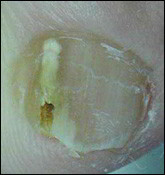
– The nail corner separates from the nail bed, looks thicker and has a whitish or yellowish colour. When scraping under the nail, one can find a whitish contagious powder. It is sometimes possible to see a kind of yellowish brown trail forming a strip or a “rocket” on the nail.
– Much more rarely, a black strip or spot which deserves immediate attention.
– White spots.
Mycoses caused by yeast
– These fungal infections essentially affect fingernails. The fungi contaminate a nail deteriorated by overexposure to moisture.
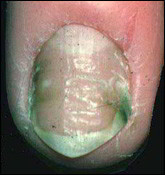
– Here again, the nail separates from the nail bed and under the nail, there is a little of a creamy white-yellowish coating. The nail may have taken on a greenish colour because of a concomitant proliferation of bacteria forming a green pigment.
– The base of the nail is inflamed and forms a red and painful roll of flesh, as well as sometimes also an undulation of the nail, causing a separation of the nail.
Mycoses caused by moulds (rare) can involve:
– A separation and thickening of the nail.
– The base of the nail is inflamed and forms a reddish and painful roll of flesh.
– White spots.
|
|||
|
|||
How is fungal nail infection diagnosed ?
A fungal culture MUST be performed to diagnose a mycosis of the nail. Indeed, even the best specialists cannot tell an onycomycosis from another nail condition with certainty. A wrong diagnosis can involve the useless and prolonged taking of expensive and potentially dangerous (or worse) drugs and prevent diagnosis of a more serious disease. Only specialized laboratories are able to proficiently perform a fungal culture, which needs to be done a certain period of time after the end of an antifungal treatment (one must wait for at least three months following the use of an antifungal lacquer or other antifungal oral medication). When correctly performed, the fungal culture can be a little unpleasant but not actually painful. Generally, the doctor needs to cut out the separated nail as far as he can to scrape underneath and reach the powdery debris. In the presence of white spots, it is necessary to scrape the surface of the nail with a blade to take the sample. Results will be available within a month.
Nail biopsy
This examination is more rarely used to diagnose nail mycosis. It may however be required in some difficult cases.
What are the treatments available for fungal nail infections ?
– Treatment of the affected nail with a 40% urea paste (Amycor-Onychoset® is available in Europe). One daily application of this ointment on the affected nail, then a bandage. Every morning, remove the debris with a spatula. This treatment will last on average from two to four weeks. If the nail is not totally disintegrated by the end of this treatment, it will need to be cut with appropriate clippers. This treatment can then be supplemented by an antifungal crearn (and a bandage) or an antifungal treating lacquer until complete recovery (two to six months).
– Application of an antifungal treating lacquer on the affected nails. According to the products, daily (Ciclopiroxolamine based nail lacquer: Penlac ® or Mycoster Lacquer@) or weekly (Amorolfine based nail lacquer) application will be required for two to six months.
It is sometimes required to have the nail surgically removed
In certain cases, the big toenail will have to be removed, in cases, for example, of mould-related onychomycosis or failure of a suitably led treatment.
An oral treatment is often necessary
As soon as the mycosis is a little advanced, a prolonged oral treatment is often required. In France, oral treatment generally consists of Terbinafine (Lamisil, one 250 mg tablet per day for 6 weeks to 6 months according to the cases). This treatment does have some side effects, usually minor (digestive disorders, skin rash), sometimes problematic (temporary loss of taste) and more rarely serious (drug-induced hepatitis, skin rash, blood anomalies or hypersensitivity). Itraconazole (Sporanox®) or Fluconazole (Flucan®), are good second line treatment options.
Combination of a topical and systemic treatment is sometimes recommended.
Frequently Asked Questions about fungal nail infections
Can a fungal nail infection mimic other diseases ?
– Fungal nail infections can look like a majority of other nail diseases. This is the reason why a fungal culture is required before starting any treatment.
– Nail anomalies consecutive to frictions are very often interpreted as being fungal nail infections, in which case an antifungal treatment is ineffective.
How frequent are nail fungal diseases ?
– Fungal nail infections are the most frequent forms of nail diseases, affecting ten percent of the population.
Are fungal nail infections contagious ?
– Nail fungal infections are contagious. It is therefore recommended to avoid walking barefoot and using someone else o towel.
What is the usual course of fungal nail infection ?
– A mycosis on one nail can spread to the other nails, but also to other regions of the body (between the thighs and the buttocks in particular).
How can one prevent onychomycosis or avoid relapses ?
– Avoid walking barefoot in public places (swimming pools, sauna, hammams, sports halls, the doctor’s office…).
– Heat and moisture are fostering factors. For mycosis pedis, it is necessary to avoid wearing sportrt shoes except for sports, to wear shoes with a leather inner sole, to use cotton socks and an anti-perspirant with 20% of aluminium chloride in case of excessive perspiration. For hand mycosis, avoid washing hands too often or without adequate protection (cotton or rubber gloves).
– Do not stop the treatment until COMPLETE recovery. It is also advised to watch for and treat rapidly all possible relapses, which are frequent, a crack in the interdigits being an early warning sign.
What can be expected from research on fungal nail infections ?
– Research is directed at finding new and more effective drugs but also at highlighting new routes of administration.
Professions at risk
People working in swimming pools
Employees in the building industry
The police forces
Food industry
Medical staff
Cleaning ladies
Minors
Personnel of armed forces
Nursery nurses, child care personnel
Sportsmen
|
|
Dermatophyte: A parasitic fungus causing diseases in skin, hair and nails.
Immunosuppressive: Which decreases the immune defences of the organism.
Yeast: A fungus which can involve diseases of the mucous membranes (mouth, digestive tract and genitals), of the internal organs and of the skin.
Onychomycosis: A nail infection caused by fungi.
Mould: Fungi which can only parasitize tissues or nails in very specific circumstances (separated nail, a nail damaged by a blow or by a skin disease, a deficient immune system).
AIDS: Acquired Immunodeficiency Syndrome caused by HIV (Human Immunodeficiency Virus) infection.
Cushing’s Syndrome: Disease of the pituitary gland leading to excess production of cortisone and other hormones by the suprarenal glands.
Raynaud syndrome: A disorder of blood circulation leading to pallor of extremities. Raynaud’s phenomenon results in crises where blood circulates badly in the finger and toes. Certain fingers or toes become livid, cold and painful, recoloration occurring within a variable period of time. Raynaud’s phenomenon may be isolated but can also accompany other diseases it serves to reveal.
Bibliographical references
2. Onychomycosis: fungal nail infection, more than a cosmetic problem (Patient information pamphlet from the Council for Nail Disorders, Schamburg, 1996).
| Warning: basic foot care can help prevent minor ailments from developing into serious ones. This article provides healthcare professionals with some useful guidelines to pass on to their patients concerning basic foot care. It should be noted, however, that these guidelines are intended for people with healthy feet and not for people who have diabetes or compromised circulation. Such patients should consult a foot healthcare professional for further guidance and treatment. |
Fabre dermatologie, Roche, Roche-Posay, Sandoz, Uriach S.A, Winderm.